While all care and diligence is taken by Dr Safvat to minimise or avoid complications, any surgical procedure can be associated with some general complications and/or specific complications related to the surgery you are having. Choosing a Specialist Plastic Surgeon such as Dr Safvat and having your procedure done in an accredited hospital minimises risks as does using an accredited Anaesthetist.
Some general surgical potential complications are:
• Infection that may require antibiotics (Dr Safvat prescribes all patients antibiotics after surgery to minimise this risk).
• Fluid build-up under the skin (seroma).
• Allergic reaction to dressings and other items used during the procedure.
• The formation of blood collection (haematoma) which could require additional surgery.
• Scars heal differently in different people. Some people are genetically prone to develop keloid scars. Hypertrophic scars develop when there is a complication in the healing process. Whilst not ideal, there is no threat to your health if you develop these.
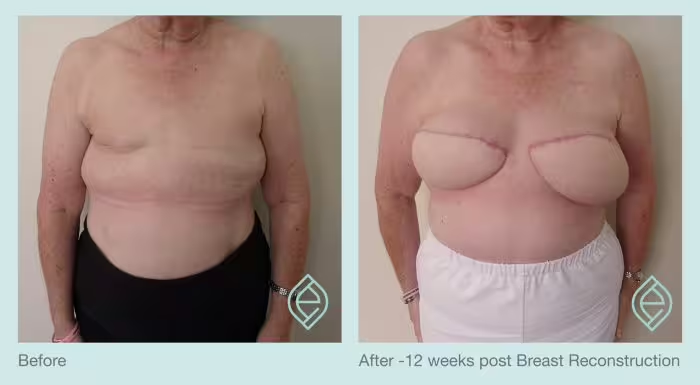
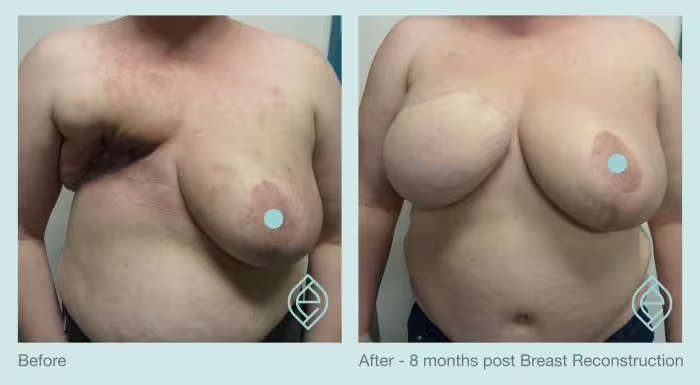
Some potential complications related to Breast Reconstruction surgery specifically are:
Alloplastic:
• Asymmetry
• Capsular Contracture (if implants are used)
• Rupture of implants due to trauma
• Changes in sensation to the breast
• BIA-ALCL (breast implant associated Anaplastic Large Cell Lymphoma)
Autologous:
• Loss of blood circulation to the reconstructed breast (causing total reconstruction loss)
• Fat necrosis (causing partial reconstruction loss)
• Asymmetry
• Changes in sensation to the breast